Increasing Vaccination: Putting Psychological Science Into Action
University of North Carolina (Brewer); Carnegie Mellon University (Chapman); University of Minnesota (Rothman); University of Sydney (Leask); University of Colorado School of Medicine (Kempe); University of Colorado Anschutz Medical Campus (Kempe); and Children's Hospital Colorado (Kempe)
"An understanding of the psychology behind vaccination behavior can inform both theoretical development and facilitation of evidence-based vaccination policy and practice."
Faced with outbreaks of vaccine-preventable diseases, parents, educators, healthcare providers, and policymakers around the world often want to know how to persuade people to get their vaccinations. But this review of the scientific findings from research on vaccination behaviour shows that the most effective interventions focus directly on shaping patients' and parents' behaviour instead of trying to change their minds.
As these researchers explain, vaccination has been shown to save lives, yet some vaccine providers and programmes face "substantial headwinds". The "public-health benefits are established or threatened by the behavior of individuals". Persistent problems include "inadequate, delayed, and unstable vaccination uptake". The "success of vaccination programmes has left people largely unaware of, and unconcerned about, diseases they have never seen and heard little about. Vaccination regularly generates controversy in traditional and social media, often because of unsubstantiated safety concerns....Program managers and providers lack evidence-based tools for effectively addressing the resulting dips in the public's confidence in vaccination....Psychology offers insight into why people engage in health behaviors, including vaccination. However, the empirical findings...appear in disconnected literatures across psychology, public health, medicine, nursing, sociology, and behavioral economics". This paper seeks "to integrate this scattered literature and to better understand how the findings inform and constrain psychological theories when applied to vaccination". It is hoped that the interventions identified, "through analyzing the psychological processes involved and reviewing the evidence, can aid policymakers and program managers as they work to improve vaccination coverage".
Psychological theories offer 3 general propositions for understanding and increasing vaccination:
- "The first proposition is that thoughts and feelings motivate getting vaccinated, yet the veracity of this claim is not well established. For instance, it makes intuitive sense that people get vaccinated because they feel at risk. But is this true? And if so, do interventions that can increase risk perceptions lead to higher rates of vaccination?"
- The second is that "the social context of vaccination has a large impact on uptake. A new mother in a parenting group who hears that her peers are getting vaccines for their children might become more inclined to do the same. But do studies support this intuition?"
- A third is that "it is possible to use psychological principles to increase vaccination directly without modifying people's thoughts, feelings, or social experiences. For instance, structuring the decision to get vaccinated as the default behavioral option is promising, but we do not know which forms of defaults are most effective and under what conditions."
The review examines the evidence for, and implications of, these 3 propositions by looking at psychological principles as applied to understanding and increasing vaccination coverage. Supply-side issues that affect vaccination coverage in many countries are not the focus of the review.
The first section situates vaccination in a public health context. It reviews the basics of vaccination, identifies the 3 main problems facing vaccination, and discusses the role of vaccination activists. One note: "Getting vaccinated is a behavior that appears simple but is actually the result of a complex series of behaviors, all of which are contingent on an interlocking system of people, funding, policies, and permissions....Studying vaccination means also studying a myriad of underlying behaviors by these various actors."
The following sections examine the evidence for the 3 psychological propositions about vaccination and their implications for intervention strategies for increasing uptake.
- Section 2 "reviews what people think and feel about vaccination and implications for behavior". The researchers "see risk appraisals, confidence, motivation, and behavior as distinct and separable constructs. These distinctions and their causal ordering are similar to several theories of behavior, such as the theory of planned behavior and the theory of reasoned action....Furthermore, the models suggest that risk appraisals and confidence in vaccination can increase motivation to get vaccinated, which in turn leads to increased vaccination." The researchers examine each of these constructs. One note: "Although health-care provider recommendations are influential, psychological science has not yet fully explained why they motivate vaccination uptake. Any of the mechanisms described in this section on thoughts and feelings can provide reasonable explanations. If a provider recommends HPV [human papillomavirus] vaccination, it may cause people to see the hazards as more likely and severe or to see themselves as more susceptible. A recommendation could increase beliefs in the vaccine's safety and reduce concerns about harm. Any of these changes would presumably increase motivation to get a vaccination."
- Section 3 "examines social processes in the context of vaccination". Vaccination is "an inherently social activity because it takes place in the context of human interactions, and receiving a vaccination (or not) affects the health of others." This section examines the influence of social interactions on vaccination. There are 4 central themes in this section:
- Social dyads, such as the relationship between patient and provider. "Patients most often obtain vaccinations from their health-care providers, and consequently the trust relationship between providers and patients is paramount....[T]he way in which providers and patients interact has critical implications for vaccination adherence. Another important social dyad is parents and children."
- Social networks, which "play an important role in vaccination attitudes and behavior. Individuals may confer with family members, friends, and members of their social network about vaccination attitudes, making vaccination decisions a part of their social identity."
- Social norms - "[p]eople tend to fit their actions to the behaviour and expectations of others, and vaccination is no exception...Health providers' own vaccination behavior, and how they propagate social norms about vaccination among their colleagues, is important..."
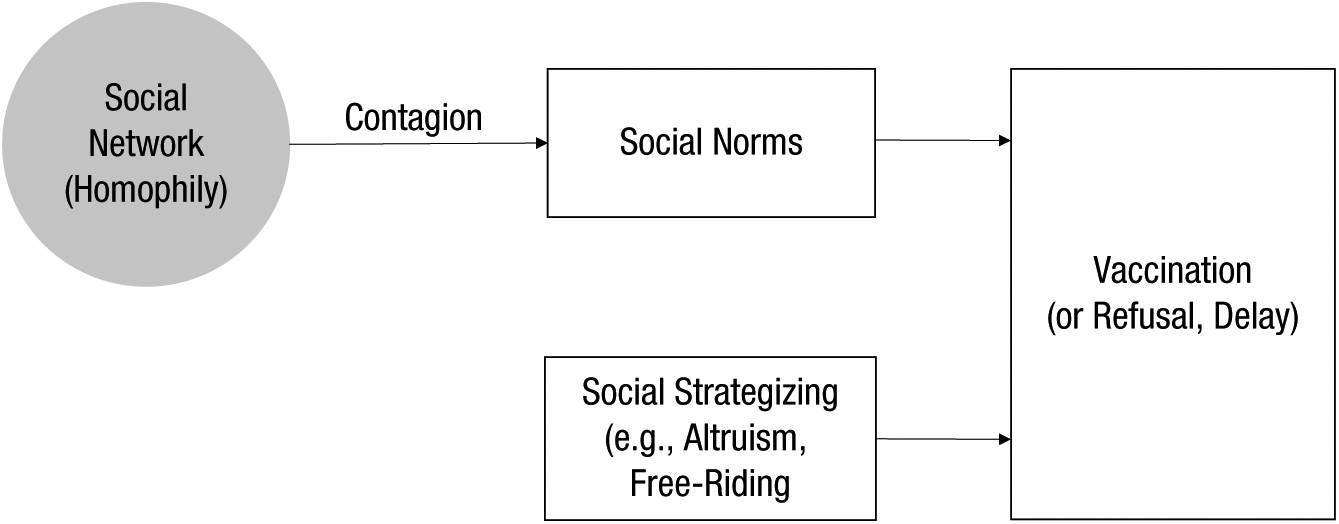
- Strategic behaviour - "[v]accination affects health at the population level because it protects the unvaccinated through herd immunity. As a result, strategic motivations to shield others from infection (i.e., altruism) can drive vaccination behavior, and the temptation to take advantage of the protection provided by others (i.e., free riding) can deter vaccination."
Also, with regard to social media, "[t]heories reviewed in this section on social processes make... predictions - for example, that when people opposed to vaccination connect on social media (homophily), it should further polarize their opinions (contagion)....Personal stories are some of the most penetrating content spread on social media....[A] large body of research in psychological science has demonstrated that anecdotes and personal stories are more influential than base rates and statistics....Recently, provaccination efforts have tried narrative approaches. For example, the U.S. [United States] National HPV Vaccination roundtable...created a series of videos with survivors of HPV-related cancers. No data are available on how these personal stories affect vaccination behaviour, which is an important opportunity for future research." Other areas for future research include "examining the spread of rumors compared with the spread of credible information on social media and how social media affects vaccination attitudes and behavior...Opportunities for intervention include social-media studies that expose people to social networks with provaccination views. Other avenues for further exploration include examining how citizen activists can use social media to build support for vaccination. Finally, social media has helped antivaccination activists to find one another and to spread their message. Understanding the nature of these messages, and helping provaccination activists to use similar methods, is an imporant opportunity....[T]he social-network and social-norm effects reviewed in this section are likely to play out on social media at least as much as in interactions that occur in-person."
- Section 4 examines approaches to changing vaccination behaviour directly, finding that "Interventions to encourage vaccination are remarkably effective when they intervene on behavior directly without trying to change individuals' thoughts and feelings about vaccination or the social context in which vaccination occurs." This section examines 3 broad groupings of intervention strategies:
- How to close the intention-behaviour gap, "present when people hold favorable vaccination intentions yet fail to act....A variety of strategies have emerged to bridge...[this] gap", such as by "keeping favorable intentions in mind through reminders, prompts, and primes and reducing barriers through logistics and healthy defaults." The researchers "consider whether these strategies can, or have the potential to, help people translate their intentions to be vaccinated into action."
- "[S]trategies designed to shape people's behavior without relying on their beliefs about vaccination". The focus is on programmes that "tie incentives or sanctions to vaccination behavior and strategies that minimize opportunities for deliberation by requiring vaccination to obtain a desired outcome (e.g., access to education or employment)."
- "[N]ew directions in research that could inform the development of new strategies to change behavior directly....In many behavioral domains, public-health programs directed considerable effort to help people develop healthy routines such that the desired behavior occurs automatically in response to cues or reminders in the situation." The researchers "consider the implications of whether getting vaccinated can become a behavioral routine and how to render aspects of the underlying behavioral process routine."
"The final section summarizes which of these psychological propositions have the greatest potential to increase vaccination coverage and how and when to deploy interventions based on them." In particular, the researchers "conclude that the most effective current methods for facilitating vaccination intervene on behavior directly, rather than attempting to change what people think and feel or their social context."
They also reiterate a theme that runs throughout the analysis: "Provider recommendation is a strong motivator for getting a vaccination across all vaccines studied. For example, in one study, 38% of adolescent boys received...[an HPV] vaccine if their parents received a provider recommendation, but only 2% received the vaccine if the parents did not receive a recommendation (Reiter, Gilkey, & Brewer, 2013; Reiter, McRee, et al., 2013)....[S]ome approaches, such as presumptive recommendations, are even more effective than standard recommendations (Brewer et al., 2017)." The researchers suggest that "[d]eveloping a better understanding of why and when provider recommendations increase vaccination could make them more effective."
The researchers find that the most effective vaccination interventions build on these favourable intentions, employing behavioural strategies to:
- Facilitate action by providing patients with reminders and prompts.
- Reduce barriers by setting default orders and appointments.
- Shape behaviour by developing incentives, sanctions, and requirements.
These conclusions are supported by multiple sources of evidence, but the researchers note that much of "the available research on vaccination behavior is limited in quality or quantity". Studies investigating vaccination attitudes and behaviour over time are rare, and few studies examine the specific mechanisms or components that make for effective interventions. They say, "We suspect that the poor performance of communication interventions reflects a reliance on a generally weak intervention approach that is grounded on interventionists' misplaced confidence that facts are persuasive and an underestimation of the impact of affect-eliciting messages such as personal testimonials."
Psychological Science in the Public Interest 2017, Vol. 18(3) 149-207. https://doi.org/10.1177/1529100618760521- sourced from: Dietrich College of Humanities and Social Sciences News, April 5 2018.
- Log in to post comments












































