Attitudes Towards Vaccines and Intention to Vaccinate against COVID-19: Implications for Public Health Communications
University College London
"...there is an urgent need for a more updated and nuanced understanding of attitudes towards vaccines and factors determining vaccine intent in the context of the COVID-19 pandemic in order to tailor public health messaging accordingly..."
Findings from nationally representative studies in the United Kingdom (UK) and Europe suggest that unwillingness and uncertainty about receiving a COVID-19 vaccine will be a significant challenge in achieving the vaccination coverage required for population immunity. This study examined predictors of vaccine attitudes in the UK, how these attitudes in turn relate to an unwillingness to vaccinate in the later context of the COVID-19 pandemic, and what these findings mean for communicators.
Cross-sectional data were collected at the beginning of a second wave of the COVID-19 pandemic (September 2020) from 32,361 adults taking part in the University College London (UCL) COVID-19 Social Study, an exploration of pandemic-related psychological and social experiences of over 75,000 adults in the UK. Ordinary least squares regression analyses examined the impact of socio-demographic and COVID-19-related factors on 4 types of negative vaccine attitudes: mistrust of vaccine benefit, worries about unforeseen effects, concerns about commercial profiteering, and preference for natural immunity. Multinomial regression examined the impact of socio-demographic and COVID-19-related factors, negative vaccine attitudes, and prior vaccine behaviour on uncertainty and unwillingness to be vaccinated for COVID-19.
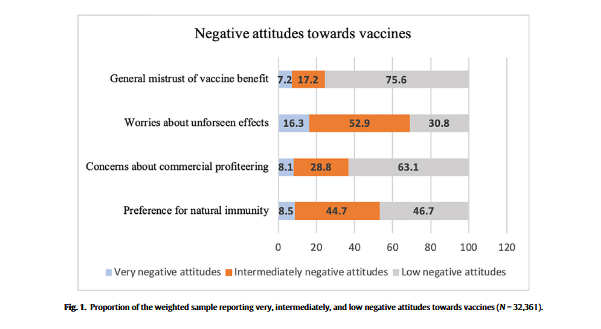
The study found that 16% of respondents displayed high levels of mistrust about vaccines across one or more domains. Distrustful attitudes towards vaccination were higher among individuals from ethnic minority backgrounds, with lower levels of education, lower annual income, poor knowledge of COVID-19, and poor compliance with government COVID-19 guidelines.
Overall, 14% of respondents reported unwillingness to receive a vaccine for COVID-19, while 23% were unsure. The largest predictors of both COVID-19 vaccine uncertainty and refusal were low-income groups (< £16,000, a year), having not received a flu vaccine last year, poor adherence to COVID-19 government guidelines, female gender, and living with children.
Amongst vaccine attitudes, intermediate to high levels of mistrust of vaccine benefit and concerns about future unforeseen side effects were the most important determinants of both uncertainty and unwillingness to vaccinate against COVID-19.
This research suggests that while certain factors predict unwillingness but not uncertainty (such as education, age, and living in a rural location), it is difficult to isolate those groups who are merely uncertain. This means that public health campaigns aimed at increasing COVID-19 vaccine uptake should focus on educating and increasing trust in both those who are uncertain and those who are unwilling with regard to: the safety, efficacy, and side effect profile of vaccines, the importance of complying with social distancing guidelines, and the virus and disease itself. Together with prior work, these findings suggest a need to tailor such campaigns to sub-groups such as those from lower socio-economic backgrounds, women, and people from ethnic minority groups. However, the researchers suggest that broader public health campaigns to include those who are already willing may also be beneficial in helping them to engage more effectively when they encounter misinformation.
Given that the results showed a relationship between low trust in government and concerns around the safety of the vaccine, the researchers suggest that communications around the vaccine should be also undertaken by groups other than those such as the European Centre for Disease Prevention and Control (ECDC). For example, at the community level, interventions involving online platforms that provide corrective factual information on vaccines and training programmes for community leaders who already have the trust of members of the public (e.g., religious leaders and community groups) to advocate for vaccination could be pursued in order to correct misinformation and improve vaccine uptake. Online educational interventions and dialogue-based interventions in healthcare settings targeting misinformation and vaccine safety have been found promising for building confidence and reducing vaccine hesitancy. The researchers suggest that there may also be a role for engaging with celebrities and social media influencers to normalise uptake of the vaccine.
"Above all, it is important that the concerns of individuals expressing hesitancy or unwillingness to vaccinate are not dismissed. Given that one of the largest predictors of vaccine hesitancy and unwillingness was misinformation about vaccines, a dialogue needs to be established with those groups to identify their specific concerns and help provide information and reassurances to break down existing barriers to intent to vaccinate."
In conclusion, the researchers suggest that "[n]egative attitudes towards vaccines are a major public health concern in the UK. General mistrust in vaccines and concerns about future side effects in particular will be barriers to achieving population immunity to COVID-19 through vaccination. Public health messaging should be tailored to address these concerns and specifically to women, ethnic minorities, and people with lower levels of education and incomes."
The Lancet Regional Health - Europe (2020), https://doi.org/10.1016/j.lanepe.2020.100012.
- Log in to post comments












































