Knowledge, Attitudes, Practices and Willingness to Vaccinate in Preparation for the Introduction of HPV Vaccines in Bamako, Mali
GAIA Vaccine Foundation (DeGroot, Rochas, Beseme, Yekta); Institute for Immunology and Informatics (iCubed), University of Rhode Island (DeGroot); Foundation GAIA (Tounkara); Regional Director of Health, Bamako, Mali (Diallo); University of Maryland School of Medicine (Tracy); Hôpital Gabriel Touré (Teguete); University of Science Techniques and Technologies of Bamako, or USTTB (Koita)
"HPV vaccination is desired and would be accepted by the vast majority of participants in this study."
Nearly 85% of worldwide cervical cancer (CC) cases diagnosed each year occur in low-resource countries; in West Africa, CC is the second most common and lethal cancer among women. Although screening for pre-cancerous cervical lesions and human papilloma virus (HPV) vaccination are accepted and effective means to prevent CC, at the time this study was performed (2011-2013), HPV vaccine was not available in Mali, but plans were underway to bring it there. Acceptance of vaccination is dependent on many factors, such as individual knowledge, beliefs about susceptibility, perceptions of vaccine effectiveness, family and physician perspectives, sexual and cultural practices, and anticipated costs of vaccination. This study therefore assessed knowledge, attitudes, and practices regarding CC and HPV among teenagers and adults living in two urban regions of Bamako, Mèkin-Sikoro and Djikoroni - both before and after a brief educational session.
The research involved 301 participants (male and female, adults and adolescents aged 12-17) in a house-to-house survey. After the study purpose was explained and informed consent obtained, the first questionnaire was submitted to the participants to assess: knowledge, attitudes, and practices; vaccine acceptability; willingness to participate in an HPV vaccination programme; and vaccination decision-making capacity. A brief information and education session took place after the first interview, consisting of information about HPV and CC, their symptoms and causes, and the availability of CC testing in Mali. A second questionnaire was then administered to measure immediate information retention and comprehension from the education session.
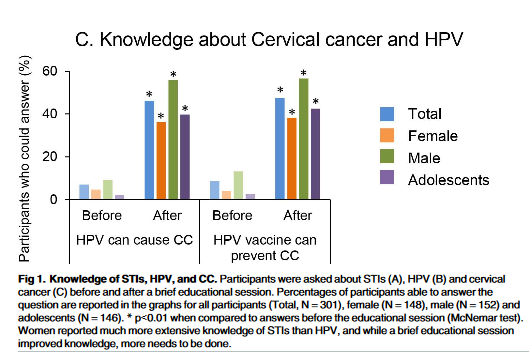
Prior to the education session, overall knowledge of HPV infection and CC was very low: Only 8% knew that HPV is a sexually transmitted infection (STI). Perhaps this is due in part to the finding that less than 20% of women had ever consulted a gynaecologist, and less than 3% had ever had CC screening. The knowledge of the participants significantly increased after the education session. Notably, all participants who knew that HPV was a STI correctly said that HPV vaccination could prevent CC. On average, the number of participants who could correctly answer the questions asked increased by 30% after the brief education session.
Vaccine acceptability was high among the participants. A majority of participants (N = 290, 96.3%) said they would like the HPV vaccine to be available in Mali, and 233 (77.4%) said they would participate in a vaccine trial. The education session increased the HPV vaccine acceptance in all groups, especially among adolescents (from 75.3% to 91.8%. Local clinics or the home were named as preferred sites for vaccination. Home visits (N = 149; 58.9%) were preferred over short messaging service (SMS) or phone calls (N = 99; 39.1%) for the purposes of receiving information about HPV vaccination appointments. This may be due to low literacy rates: Only 31% of Malians over age 15 are literate (2010 data from the World Health Organization, or WHO), meaning that 69% of the intended population would be unable to read a text message.
The results suggest that men's opinions will be an important factor to consider when implementing vaccination campaigns. Half of adult females (39, 52.0%) said they would have to ask their husband's permission before deciding to vaccinate their child. However, most adult men (88.9%) were not able to decide or would ask their parent's opinion. Only one adult male participant (1.3%) reported that he would consult his wife about HPV vaccination. Among adolescents, boys would be more inclined to ask permission from their parents, but overall they would be more involved in the decision to get vaccinated (59.7%) than girls (43.2%). "[I]nvolving men in education about prevention programs, engaging men in making positive health decisions for women and children, and including men in publicity materials will be important to promote prevention programs not only in Mali, but also in other societies where men are heavily involved in decisions about women's health."
The researchers indicate that issues that remain to be addressed to improve the situation regarding CC prevalence and limited access to CC screening in Mali and West Africa include: low levels of HPV and CC knowledge; limited knowledge about the purpose and location of CC screening, and lack of access to CC screening. They are evaluating methods for increasing participation in HPV/CC screening using community education sessions and a patterned cloth as a visual teaching tool.
They write, "It is clear from this study that HPV vaccination campaigns should be carefully structured, taking into consideration local cultural norms. Autonomy regarding vaccination was low among women and girls, thus, future studies should examine whether HPV vaccination campaigns should be conducted in clinical settings or at home, and how decisions about HPV vaccination, that are made in consultation with fathers or husbands, could be facilitated."
PLoS ONE 12(2): e0171631. doi:10.1371/journal.pone.0171631
- Log in to post comments












































