Questions and Concerns About HPV Vaccine: A Communication Experiment
Fred Hutchinson Cancer Research Center (Shah); University of North Carolina (Shah, Gilkey, Boynton, Dailey, Todd, Robichaud, Margolis, Brewer); Pennsylvania State University (Calo); Penn State Cancer Institute (Calo); SAFEchild Advocacy Center (Todd)
To date, randomised control trials (RCTs) have identified communication techniques providers can use to broach the topic of human papillomavirus (HPV) vaccination and make effective recommendations to parents. However, few studies have focused on how providers can successfully address questions and ease concerns parents may have after the initial recommendation. Thus, these researchers conducted an online video-messaging experiment with parents of preteenagers and teenagers to identify messages that providers can use to address common parental questions and concerns about HPV vaccine and to identify characteristics of messages that explain their greater efficacy.
Participants in the study were members of an existing national online-probability panel of 55,000 United States (US) adults. Eligible respondents were parents of at least 1 child aged 9 to 17 years who either had not initiated the HPV vaccine series or had received only the first dose. From November 2017 to January 2018, the researchers surveyed 1,196 of these parents. Parents were exposed to 2 different video-messaging experiments during the survey. In the first experiment, the researchers randomly assigned all parents to conditions by employing different vaccine recommendation strategies. In the second experiment, they randomly assigned all parents to messages in which questions or concerns about different HPV vaccine topics were answered.
The survey software randomly assigned parents to receive video messages about 1 of 7 topics about HPV vaccine that parents had reported wanting to learn more about (e.g., recommended age). Once randomly assigned, parents watched 4 prerecorded video messages about that topic in random order, all of which were delivered by a board-certified female paediatrician. After each video message, the survey asked parents questions, including, "How much would hearing your doctor or health care provider say this increase your confidence in the HPV vaccine?" and "How much would hearing your doctor or health care provider say this make you want to get the [next dose of the] HPV vaccine for your child?"
Most parents wanted to talk with their children's healthcare providers about the 7 HPV vaccine topics, ranging from 68% who wanted to talk about safety and side effects to 84% who wanted to talk about the diseases prevented by HPV vaccine. Parents placed the lowest priority on discussing vaccination for boys and girls (8%), vaccination for children who were not sexually active (7%), school requirements for vaccination (6%), and national recommendations for HPV vaccine (5%).
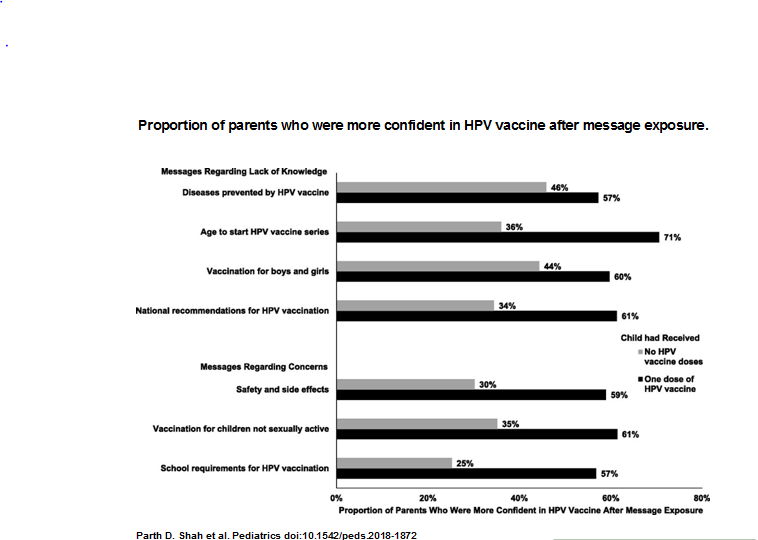
Among parents whose children had not yet received HPV vaccine, the proportion who were moderately or a lot more confident in HPV vaccine after message exposure ranged from 25% to 46%. Confidence was highest after the parents were exposed to messages about the diseases prevented by HPV vaccine (46%) and vaccination for boys and girls (44%). Confidence was lowest after parents were exposed to messages about safety and side effects (30%) or school requirements for HPV vaccination (25%). Among parents of children who had initiated the HPV vaccine series, the proportion of those who were more confident in HPV vaccine after message exposure ranged from 57% to 71%. Confidence was highest after parents were exposed to messages about the age to start HPV vaccination (71%). For the other topics, approximately three-fifths of parents were more confident after message exposure.
The study found that parents were more confident in HPV vaccine when they were exposed to messages that addressed lack of knowledge about HPV vaccine (b = 0.13; P = .01), messages that included information about cancer prevention (b = 0.11; P .001), messages that required a higher reading level (b = 0.02; P = .01), and messages that were longer (b = 0.03; P .001). Parents were less confident in HPV vaccine when exposed to messages in which urgency was expressed (b = -0.06; P = .005). Analyses conducted by using HPV vaccine motivation as an outcome revealed the same pattern of findings.
Thus, this study offers research-tested messages that providers can use to address parents' HPV vaccination questions and concerns about 7 common topics. General communication principles for increasing message effectiveness are to include information on the benefits of vaccination (including cancer prevention) and avoid expressing urgency to vaccinate when addressing parents' questions or concerns. Brief messages that address common questions and concerns can boost the confidence of parents with children who have initiated HPV vaccination. However, providers may need to be prepared to have longer conversations with parents who express concerns about HPV vaccine, especially regarding safety and side effects. Patients in other studies have reported finding value in receiving additional information, such as from fact sheets, and in participating in motivational interviewing. As a means of conveying complex information about HPV vaccination, providers may consider using validated visual aids in their conversations with parents,36 particularly those who may have lower levels of health literacy.
Seven brief messages that providers can use to address parents' questions and ease concerns are shown in Table 5 in the paper. The researchers consider them to be effective messages in eliciting confidence and motivation for each HPV vaccine topic. They adjusted the messages in places to align with the previously described communication principles. Providers may take these messages as a starting point and elaborate as needed.
Pediatrics. 2019;143(2):e20181872
- Log in to post comments












































