Parental Hesitancy About Routine Childhood and Influenza Vaccinations: A National Survey
University of Colorado and Children's Hospital Colorado (Kempe, Saville, Helmkamp, Dickinson); University of Colorado (Kempe); University of California at Los Angeles Mattel Children's Hospital and University of California at Los Angeles (Albertin, Breck, Szilagyi); Indiana University (Zimet); University of California at Los Angeles (Vangala); University of Rochester (Rand); Children's Mercy Kansas City (Humiston)
"...underscore the importance of better communicating to providers and parents the effectiveness of influenza vaccines in reducing severity and morbidity from influenza, even in years when the vaccine has relatively low effectiveness..."
Although yearly influenza vaccination is recommended for all children 6 months to 18 years, the influenza vaccination rate for United States (US) children in the 2018 to 2019 season was only 57.9%. In an attempt to assess the degree to which hesitancy - "a motivational state of being conflicted about or opposed to getting vaccinated" - contributes to this low rate, the researchers conducted an online survey of a nationally representative sample of US parents in February 2019.
Among the 2,176 parents who completed the survey, the researchers assessed hesitancy using a modified 5-point Vaccine Hesitancy Scale (VHS) and labeled parents as hesitant if they scored higher than 3.
Hesitancy prevalence was 6.1% for routine childhood and 25.8% for influenza vaccines. Regarding routine childhood vaccines, among hesitant respondents, 67.5% had deferred or refused routine vaccination for their child because of concerns about that vaccine, compared with 8.7% of nonhesitant parents. Regarding influenza vaccine, among hesitant respondents, 70.1% had ever deferred or refused influenza vaccination for their child because of concerns about that vaccine, compared with only 10.0% of nonhesitant respondents.
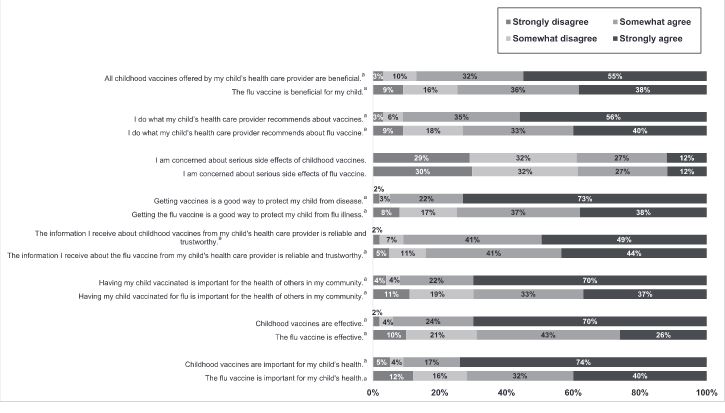
The item most associated with hesitancy about childhood vaccines was having concerns about serious side effects, with 12% strongly and 27% somewhat having this concern.The percentages of parents who were strongly or somewhat concerned about serious side effects of influenza vaccine were identical to those seen for routine childhood vaccines. However, only 26% strongly agreed that the influenza vaccine is effective, compared with 70% for childhood vaccines (P < .0001). Parents were also less likely to perceive influenza vaccines as important for their child's health, to agree that influenza vaccines are beneficial and a good way to protect their child from disease, and to report doing what their child's health care provider recommended regarding influenza vaccines.
In multivariable models, an educational level lower than a bachelor's degree and household income <400% of the federal poverty level predicted hesitancy about both routine childhood and influenza vaccines. Hispanic parents were less hesitant about influenza vaccines than white, non-Hispanic parents. Having more children in the household and being an unmarried respondent were also associated with hesitancy about influenza vaccines.
Thus, vaccine hesitancy, particularly for influenza vaccine, is prevalent in the US. Hesitancy about influenza vaccination is largely driven by concerns about low vaccine effectiveness. The researchers speculate that concerns about low effectiveness may have led to other concerns found in the survey. For example, parents convinced that the influenza vaccine is ineffective might also deny that it is "important for the health of others", "important for their child's health", or "a good way to protect my child from disease” and might be less likely to do "what my child's health care provider recommends about flu vaccine". Confidence in influenza vaccine effectiveness may have been eroded during well-publicised influensa seasons during which there was a significant mismatch between circulating and vaccine strains of influenza. Poor live attenuated influenza vaccine effectiveness, with removal of the vaccine from Advisory Committee on Immunization Practices recommendations during 2 seasons, also may have eroded confidence in influenza vaccine's effectiveness.
In view of these findings, what methods can be used to increase decisions to vaccinate among parents who are hesitant? Evidence is strongest for methods that build on whatever favourable intentions to vaccinate exist or those that focus on changing behaviour directly rather than trying to change beliefs or attitudes. Such interventions would include strong and presumptive (rather than open-ended) recommendations by a trusted provider, among others. There is evidence that communication techniques such as motivational interviewing can be helpful in convincing some hesitant parents to vaccinate in the primary care setting. The use of social media interventions, some of which involve trained parents as advocates for vaccination within their own communities, have shown some effectiveness in overcoming hesitancy. "Quantifying the level of hesitancy nationally on a longitudinal basis by using a consistent measure is a critical first step in guiding and measuring the effectiveness of future interventions to counter vaccine hesitancy."
Pediatrics July 2020, 146 (1) e20193852; DOI: https://doi.org/10.1542/peds.2019-3852
- Log in to post comments












































