Increasing Immunisation in Ogun State, Nigeria: A Formative Evaluation of a Participatory Action Research Intervention
Royal Tropical Institute (Akwataghibe); Ogun State Primary Health Care Development Board (Ogunsola); University of Ibadan (Popoola); Morgan State University (Emeji)
"Can a PAR approach be used to strengthen community links in the REW strategy in order to facilitate an increased uptake of immunization in Ogun state of Nigeria?"
In 2005, Nigeria adopted the Reach Every Ward (REW) strategy to improve vaccination coverage for children 0-23 months old through community mobilisation and outreach conducted by health facilities to under-served or hard-to-reach areas. By 2015, Ogun State in the southwestern region had achieved full immunisation coverage in 12 out of 20 of its local government areas (LGAs). However, the remaining areas continued to face barriers to achieving full immunisation coverage, with the highest proportion of unimmunised children belonging to the Remo North LGA. A participatory evaluation and participatory action research (PAR) approach was introduced to provide context-specific solutions to increase immunisation coverage in Remo North. This International Initiative for Impact Evaluation (3ie) report shares the formative evaluation of the PAR intervention.
The rationale for the strategy was that using methods that involve iterative processes of reflection and action carried out jointly with communities, health workers, and local government officials could provide insight into the community-related factors that hinder immunisation coverage, in response developing realistic, context-specific solutions. A common ideology in all designs of PAR is that research and action must be done "with" people and not "on" or "for" people. Through self-reflective enquiry carried out by participants in group settings, the PAR approach is based on empowering diverse local people to voice their opinions and join in decision-making to address challenges in implementing locally relevant actions for change and in monitoring and evaluation of change.
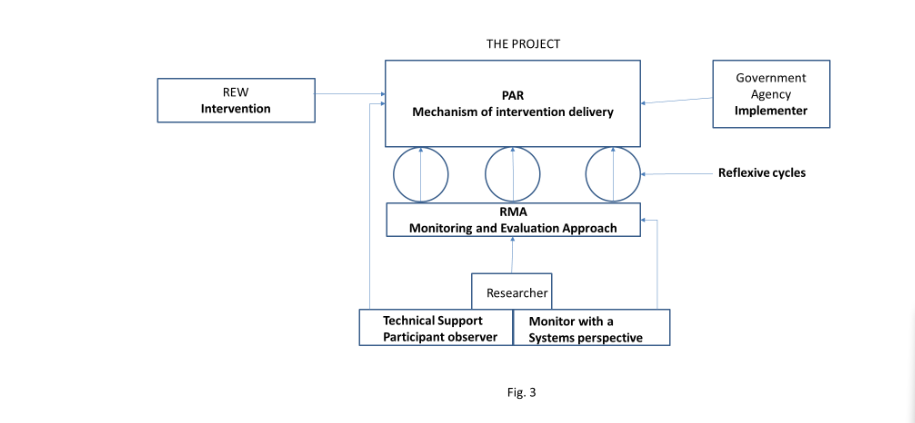
The PAR took place in 2016-2017 and is described in detail in the body of the report and in its annexes. In brief, the PAR commenced with a baseline study using both quantitative and qualitative methods. This situational analysis informed the first round of dialogue among community members, health workers, and local government officials to develop a Joint Action Plan (JAP), which was implemented over 4 months. Researchers then assessed progress, which informed a second round of dialogue. The participants developed a second JAP, which was again implemented over 4 months. This process aimed at addressing the social (relating more to the community members) and structural (relating more to health system factors) determinants influencing immunisation coverage. Reflexive Monitoring in Action (RMA), an approach developed by researchers in Wageningen University and the Vrije University Amsterdam in the Netherlands, was used throughout the project's cycles, providing a platform for several reflective cycles of learning and evaluation between researchers/evaluators, communities, health workers, and local government.
A pre-test/post-test study was carried out in Remo North's Ipara and Ilara wards, the best- and worst-performing wards in terms of immunisation coverage. Quantitative methods included a household survey (HHS) for caregivers, a secondary analysis of the National Health Management Information Systems (NHMIS) data, and a cost-effectiveness analysis of the PAR approach. Qualitative methods included in-depth interviews and focus group discussions with policymakers, local government officials, community leaders, health workers, PAR participants, and community members.
The evaluation found that collaboration of the community members, health workers, and local government officials resulted in the strengthening of the community links to immunisation both in Ilara and Ipara. The Ward Development Committee (WDC) in Ilara was revitalised from its defunct state at baseline. The collaboration between the Joint Action Committee (JAC) and the WDC was perceived as effective in the implementation of the JAPs. The involvement of WDC and Social Mobilization Committee (SMC) members in the dialogues and action eased the integration of the PAR into these existing community structures and promoted a sense of ownership.
A key benefit of the PAR intervention noted in this study was its value in health systems strengthening, though the PAR could not change major flaws in the system. Health facility conditions appeared during the baseline to be crucial for women to attend immunisation services. Through the PAR intervention, the community was able to revitalise the Ilara healthcare facility, which meant that the community members no longer had to travel to Ipara to access health services. Significantly more caregivers visited fixed government health facilities for immunisation services at endline (83.2%) than caregivers at baseline (54.2%) in both wards.
Immunisation coverage, assessed by card only in the HHS, increased significantly at endline (90.9%) compared with 60.7% at baseline for both wards. An assessment of the NHMIS data indicates that immunisation coverage in the Ilara ward increased from 26% to 59%. For Ipara, coverage for all the antigens except measles remained high. The significant decline in measles coverage was ascribed to persisting cultural barriers and the reduction in clientele to the Ipara healthcare facility due to revitalisation of the healthcare facility in Ilara.
Knowledge of SMC and WDC members by the caregivers in the HHS increased significantly at endline. Furthermore, the study showed that children above the age of 9 months were 3.68 times more likely to be fully immunised when caregivers were knowledgeable of SMC members (and 1.20 times more likely with knowledge of the WDC members) - indicating an important connection from the strengthening of these community links to increase in immunisation utilisation among caregivers in the communities.
Though the researchers did not see many changes in the existing power dynamics between the 3 groups, there were shifts between the Ilara community members (who now played a monitoring role in the health facility) and the health workers, who displayed increased social accountability in their availability and behaviour. Leadership of the JAC appeared to be more effective in the more cohesive and rural setting (Ilara), and conflict within the Ipara group appeared to contribute to its under-performance in the PAR. Further research into group dynamics could provide more insight into social pressure and the emerging social accountability, into the perceptions of the different representatives regarding their position and collaboration, and the relation of these new structures (dialogues) with the existing ones.
The qualitative data indicate that men were primary decision makers about who gets vaccinated within the household, as well as in the community. Decisions taken by women, including whether or not to immunise their children, had to be approved by men. During the focus group discussions, participants brought up issues regarding adverse events following immunisation (AEFI). They expressed that most people in the communities know the importance of immunisation, and yet some people refused to have their children immunised due to fear of adverse reactions. However, according to the researchers, due to community mobilisation as per the PAR action plan, there was increased sensitisation towards immunisation and its benefits in the community. A high proportion of caregivers had changed their perceptions about AEFI. The increased awareness, particularly in the Ilara community, led to a decrease in fear among the community members about AEFI, in the estimation of the researchers.
The authors recommend a full impact evaluation, with careful attention to design and a counterfactual so as to ascertain the effectiveness of the PAR intervention and its replicability.
3ie website, July 30 2019.
- Log in to post comments












































